Understanding Diabetic Ulcers: Risks, Prevention, and Timely Intervention
Diabetic ulcers are a grave concern for individuals living with diabetes. These ulcers, which can penetrate through multiple layers of skin and reach the underlying tissue and bone, often occur on the toes and balls of the feet. In this blog post, we will explore what diabetic ulcers are, the associated risks, essential precautions to take, the importance of timely treatment, and how collaboration can help prevent severe consequences.
What is a Diabetic Ulcer?
A diabetic ulcer refers to an open wound that extends through all layers of the skin, reaching the tissues beneath, and sometimes even affecting the bone. Due to neuropathy and damaged nerves, some ulcers may not be painful, leading to potential negligence in care. It is crucial to understand that these ulcers primarily afflict individuals with diabetes.
Understanding the Risks:
Neglecting a diabetic ulcer can have dire consequences. Let’s explore the risks associated with these ulcers:
- Serious Infections: An untreated ulcer can quickly become infected, which, if left uncontrolled, may lead to life-threatening complications.
- Amputation: Poor circulation resulting from diabetes increases the risk of amputation in cases where the ulcer fails to heal properly.
- Delayed Healing: Elevated blood sugar levels and excessive pressure on the foot can impede the healing process, prolonging recovery time.
- Bone Infection: Failing to address the wound promptly may result in a bone infection, further complicating the healing process and overall health.
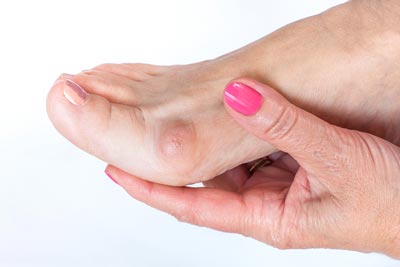 Diabetic Ulcers
Diabetic Ulcers
What NOT to Do:
To ensure the best possible outcome, it is important to avoid certain actions when dealing with a diabetic ulcer:
- Avoid Weight-bearing: Minimizing pressure on the affected area is crucial to prevent further damage and promote healing.
- Stick to Recommended Products: Only use products recommended by your doctor or healthcare professional for ulcer care.
- Recognize Signs of Infection: Do not ignore warning signs such as pain, redness, swelling, or drainage around the ulcer, as they may indicate a potential infection.
- Always Wear Appropriate Footwear: Walking without shoes increases the risk of injury and can exacerbate the condition.
Timeline Expectations:
The healing timeline for diabetic ulcers can vary significantly, ranging from a few weeks to several months. Adhering to the recommended treatment protocol and exercising patience are mission-critical. While recovery times may differ, following professional guidance and remaining committed to the healing process is instrumental in achieving positive outcomes.
The Bigger Picture:
Diabetic ulcers should never be taken lightly, as neglecting them has led to devastating consequences such as amputations and even loss of life. Prompt professional intervention and proper wound care significantly increase the chances of faster healing and reduce potential downtime. By addressing even the smallest skin opening early on, we can collectively minimize the risk of dire complications.
Managing diabetic ulcers requires proactive attention and prompt medical intervention. Understanding the associated risks, avoiding specific actions, adhering to treatment plans, and seeking early medical assistance are pivotal steps in preventing severe consequences. By prioritizing timely care, collaborating with healthcare professionals, and following best practices, we can improve outcomes and ensure a better quality of life for individuals living with diabetes. Remember, together, we can prevent dire consequences and foster optimal healing.
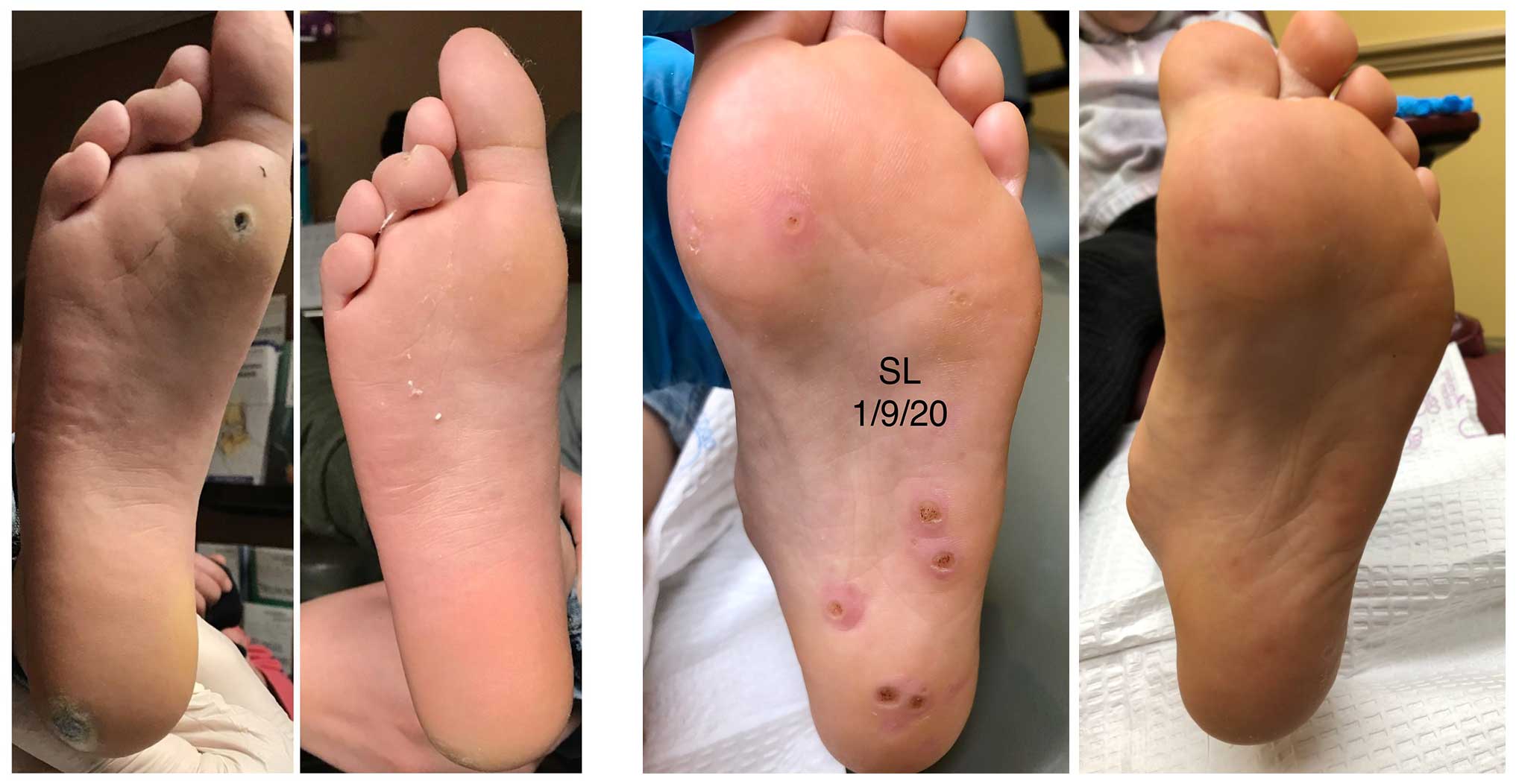 Plantar Warts
Plantar Warts
Flagstaff Foot Doctors: Anthony Rosales DPM
https://www.google.com/maps?cid=8835841318590452161
421 N Humphreys St, Flagstaff, AZ 86001, United States
(928) 774-4825
https://flagstafffootandankle.com/
